To slow the spread of Covid-19, governors in 46 states have closed more than 91,000 U.S. public and private schools, affecting more than 50 million school students. Most of the closures are currently scheduled to last for only two to three weeks (see figure). As those deadlines approach, governors now confront the difficult questions of whether to reopen schools, and if so, when?
There were three main reasons governors choose short-term closures. First, it took advantage of the spring break days already built into many school calendars. Second, guidance from the Centers for Disease Control and Prevention recommended 14 day closures in part because of studies suggesting the Covid-19 incubation period is 14 days. Third, it mandated social distancing while giving state leaders, local health officials, and superintendents the necessary time and space to evaluate the precautions.
With end dates to short-term closures fast approaching, there is little clarity about the conditions and factors that should trigger the reopening of schools. The CDC website simply states that federal health officials are “currently working on additional guidance to help schools determine when and how to re-open in an orderly manner.” As a result, we’re likely to see many states extend school closures for another two weeks or to the end of April. Kansas and Virginia have already announced that schools will remain closed for the rest of the academic year, and California governor Gavin Newsom has indicated that he may follow their example.
Statewide School Closures
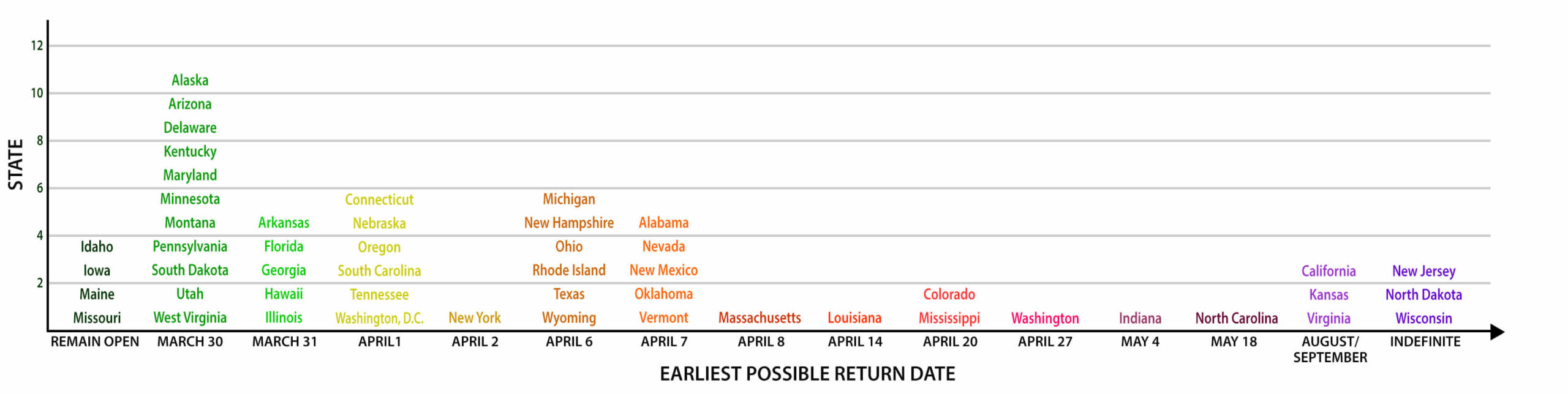
Source: Council of Chief State School Officers; Education Next research.
Notes: Nebraska closed for 6 to 8 weeks on March 17, with reviews every two weeks. March 31 would be its earliest return date.
Boston public schools are closed until Monday, April 27.
All data as of March 24, 2020.
More up-to-date closure and re-opening information, accurate as of May 4, 2020, is available here.
One reason for the lack of concrete guidance on reopening schools is that medical professionals are still racing to better understand Covid-19. The novel coronavirus is proving to be an epidemiological puzzle with many unanswered questions. How does it spread? Why has it spread so quickly in certain areas but not others? Why doesn’t the virus cause symptoms right away? Can people become re-infected with the virus after they’ve had it? Which social distancing measures affect the transmission rate? Answers to these questions will inform the use and duration of school closures as well as other strategies needed to slow transmission.
Children are also part of the mystery. Most influenza and pandemic planning assumes that children are among the most susceptible to infection and would have higher levels of mortality. That, however, isn’t the way Covid-19 is playing out. Initial data found that older adults are more susceptible but more recent data suggested that 40% of patients are actually younger (between the ages of 20-50). Children seem largely asymptomatic. A Chinese study of 2,000 confirmed childhood cases found that just over half had mild to no symptoms at all.
While children may be resistant to the most severe symptoms and complications resulting from Covid-19, they are likely to be carriers which could transmit the virus to others. As any parent or teacher knows, children are “super spreaders,” meaning that they are excellent transmitters of viral infections since they tend to not be good social distancers. They struggle with washing their hands or giving each other space. The theory behind school closures is that they cut off the virus’ line of transmission by forcing the social distancing of these super spreaders. Reopening schools too early in an outbreak could lead to children accelerating the spread of the virus.
All of these unanswered questions made it difficult to build forecasting models of the spread of Covid-19 or to estimate which social distancing measures have the greatest impact on “flattening the curve.” It also makes it difficult to determine when to relax these measures, hence CDC’s rather vague guidance:
“Available modeling data indicate that early, short to medium closures do not impact the epi curve of COVID-19 or available health care measures (e.g., hospitalizations). There may be some impact of much longer closures (eight weeks, 20 weeks) further into community spread, but that modeling also shows that other mitigation efforts (e.g., handwashing, home isolation) have more impact on both spread of disease and health care measures.”
The Imperial College of London released its own modeling study on likely U.S. and U.K. outcomes, including the effectiveness of various measures. The report paints a grim picture of millions of deaths if nothing is done. But aggressive social distancing actions, including school closures, over five months can help suppress the transmission rates and flatten the curve. The challenge is that once these measures are relaxed, the virus is likely to make a rebound, leading to a second and third wave.
Policymakers are also exploring a recommendation from the Imperial College report to fight the virus through an “adaptive policy.” The graphic designers at the Economist provide a helpful illustration to better understand this approach, which Thomas Pueyo discussed in a Medium essay titled “The Hammer and the Dance.”
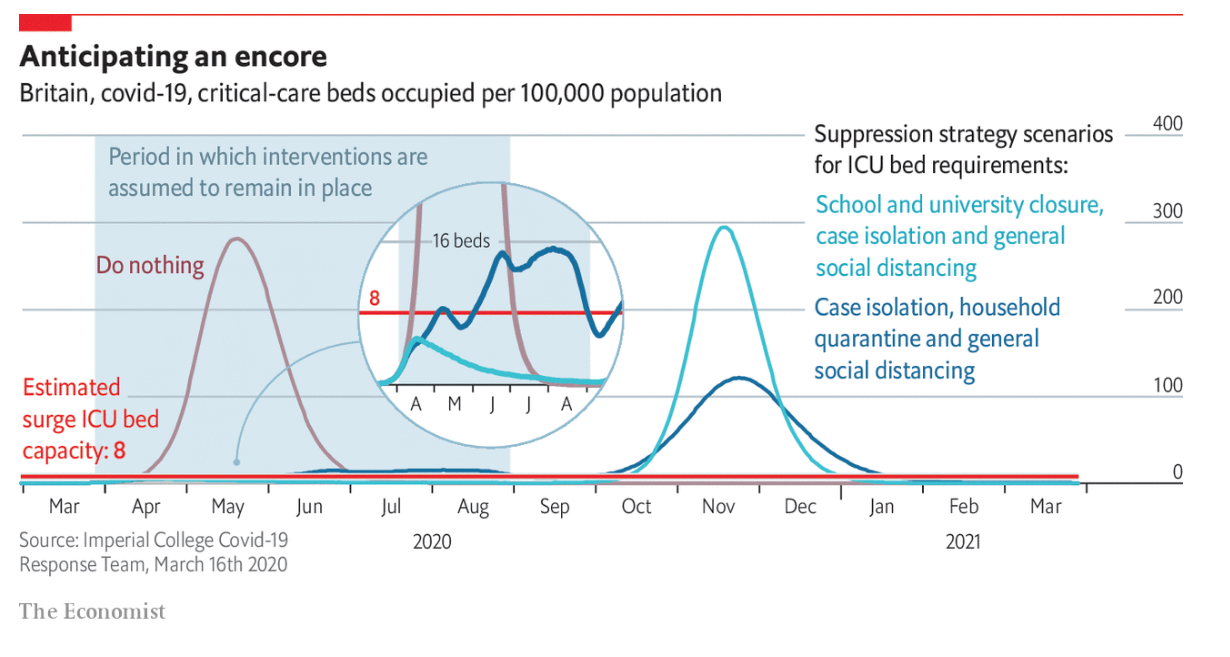
The idea is to have five months of very strict measures (school closures, social distancing, etc). At that point, some social distancing measures would be relaxed, including reopening schools for the next academic year. This model predicts that we will see a rebound of the virus next fall and winter. A trigger mechanism would then reenact stricter measures once weekly confirmed cases exceed a threshold. As a result, we could face a series of rolling, targeted school closures over the next 18 months, triggered by a spike of cases in a region.
The White House seemed to signal this approach in a press briefing on Monday, March 23. President Trump said, “In other cases…certain governors are going to maybe have a decision to make [about reopening schools]. Now, they may make a decision to keep them open — in a certain part of New York and in Westchester County or wherever it may be, they will keep them closed. But they’re going to have leeway. We are giving the governors a lot of leeway.”
But there’s a real risk of reopening schools and returning to normal life too soon. The models upon which public policymakers are basing their decisions are only as good as the data they’re based on. Unfortunately, the lack of widely available testing in the United States has deprived researchers of the data they need to run and tweak the scenarios. Both the CDC and the Imperial College models use data from cases in China, but as discussed earlier, the cases in Italy are surfacing with a much younger population. Undoubtedly other new patterns will surface in the United States which have implications for the models we use to guide policy decisions.
The lack of more compelling data has led some former officials to caution against taking more drastic actions until we have better information. In a New York Times article, Dr. Thomas Frieden, a CDC director under President Obama, was quoted as saying, “Closing all schools may not make sense unless there is documented widespread community transmission, which we’re not seeing in most of the country.” Another top federal health official in the Obama administration, Andy Slavitt, expressed even greater skepticism, “From every expert I have talked to, I am less convinced that schools should be closed.”
There is one final unknown variable. Currently, the public health benefits of school closures and home quarantining outweigh the costs. But at what point does that equation flip? When do the economic, societal, and educational costs outweigh the public health benefits of these aggressive social distancing actions? Schools and community members were quick to heed the warnings and direction of state officials with respect to social distancing. But public health officials worry about a “behavioral fatigue” when people become less vigilant and cooperative with the inconveniences and hardships they’re asked to endure.
Given the enormous uncertainty, how should school leaders and policymakers plan? If we assume that we’re not yet at the peak of the spread, then the most likely scenario is that governors will continue following CDC guidance and extend closures for another 2-4 weeks, at which point they can reevaluate. But it is just as likely that governors begin closing schools for the rest of the year, as we have seen in Kansas and Virginia.
With all of this in mind, education leaders and policymakers will need to start three parallel sets of work.
First is continuing the rapid response necessary to mitigate the loss of learning from this year’s closures. School systems have been heroic in rapidly setting up remote learning efforts, but superintendents and principals need to find ways of strengthening and improving these offerings for the remainder of the school year.
Second, leaders will need to use time over the summer to make preparations for the new academic year. There will need to be a massive amount of formative assessments when schools reopen to gauge the loss of learning and the needed interventions and supports. School districts will also need to use this time to prepare for possible closures in the fall and winter, including professional development for their teachers, deciding ahead of time the type of online resources and service they will use during closures, and also stocking up on laptops and mobile hotspots that can be loaned out to students. They can use these months also to understand and address the gaps in their school meal distribution plans.
Finally, schools will be on the front line of an adaptive policy approach next school year. Health officials rely on them as part of “disease surveillance” to track the spread of viruses. As a result, schools will need to develop testing and reporting regimens with their local and state health officials to serve as an early warning system that can inform the enactment of social distancing measures.
We are still in the early days of understanding Covid-19. Fighting it will require school leaders to develop the new strategies needed to navigate these uncharted waters.
John Bailey is an advisor to the Walton Family Foundation and a visiting fellow at the American Enterprise Institute. He previously served in the White House, U.S. Department of Commerce, and U.S. Department of Education.
Read more from Education Next on coronavirus and Covid-19.


